Scientists can see chronic pain in the brain with new clarity.
Over months, electrodes implanted in the brains of four people picked up specific signs of their persistent pain. This detailed view of chronic pain, described in Nature Neuroscience on May 22, suggests new ways of curtailing the excruciating condition.
The approach “provides a way into the brain to track pain,” says Katherine Martucci, a neuroscientist who studies chronic pain at Duke University School of Medicine, Science News reported.
Chronic pain is incredibly common. From 2019 to 2020, more American adults were diagnosed with chronic pain than with diabetes, depression or high blood pressure, researchers reported in JAMA Network Open May 16.
The pain is also incredibly complex, an amalgam influenced by the body, brain, context, emotions and expectations, Martucci says.
That complexity makes chronic pain seemingly invisible to an outsider and very difficult to treat.
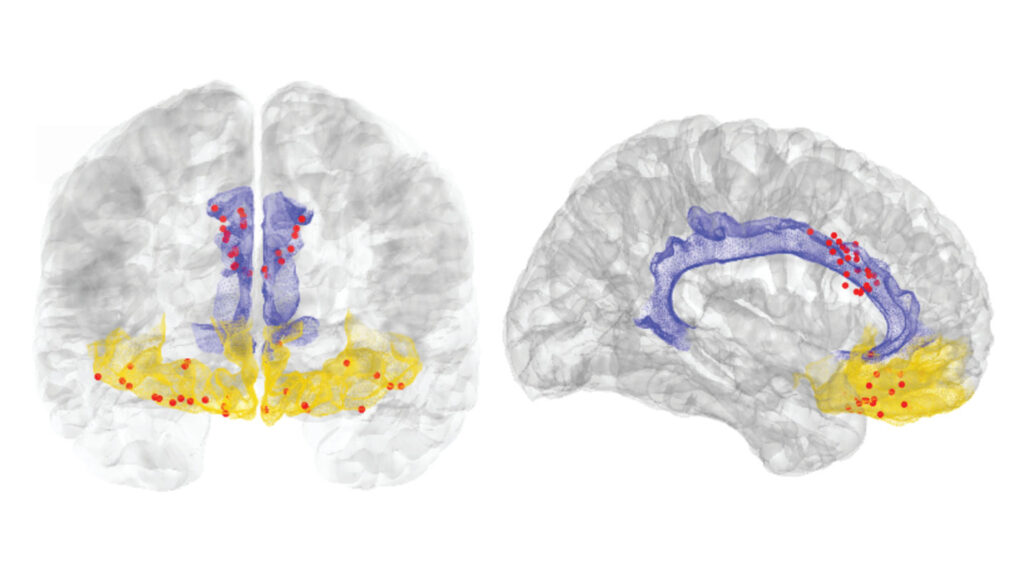
One treatment approach is to stimulate the brain with electricity. As part of a clinical trial, researchers at the University of California, San Francisco implanted four electrode wires into the brains of four volunteers with chronic pain. These electrodes can both monitor and stimulate nerve cells in two brain areas: the orbitofrontal cortex, or OFC, and the anterior cingulate cortex, or ACC.
OFC isn’t known to be a key pain influencer in the brain, but this region has lots of neural connections to pain-related areas, including ACC, which is thought to be involved in how people experience pain.
But before researchers stimulated the brain, they needed to know how chronic pain was affecting it. For about three to six months, the implanted electrodes monitored brain signals of these people as they went about their lives. During that time, the participants rated their pain on standard scales two to eight times a day.
Using sophisticated machine-learning approaches, researchers then linked each person’s pain ratings to their brain activity patterns, ultimately landing on a signature of each person’s chronic pain.
In many ways, the patterns were unique to each person, but there was overlap: Brain activity in OFC, an area at the front of the brain just behind the eyes, tracked with people’s chronic pain levels. Some unexpected pain patterns cropped up along the way, too. Two volunteers’ pain fluctuated on a roughly three-day cycle, for instance.
“Brain activity in OFC could represent a solid biomarker of chronic pain, a signal that could both help doctors track treatment responses and serve as new targets for treatment,” says neuroscientist Chelsea Kaplan of the Chronic Pain and Fatigue Research Center at the University of Michigan in Ann Arbor.
The study was done on only four people, three with pain from a stroke and one with phantom limb pain after a leg amputation.
“We would need to know if these findings can generalize to other patients and pain conditions,” Kaplan says.
If brain activity patterns end up being common across people with chronic pain, they might one day be used to measure pain in people who can’t communicate, Martucci says.
That includes people in nonresponsive states such as those with locked-in syndrome.
Yet the goal of identifying reliable markers of chronic pain is not necessarily to establish whether a person is in pain, or serve as a yes-no diagnostic test, study coauthor Prasad Shirvalkar, a neurologist at UCSF, said in a May 18 news briefing. Instead, it’s to guide treatment. Shirvalkar and his colleagues are now conducting a clinical trial that involves stimulating peoples’ brains to treat chronic pain.